Patients discharged during holiday period at a higher risk of death and hospital readmission: U of T led study
December 17/2018
by Rebecca Biason, IHPME
While many of us look forward to slowing down during the holiday season whether by lessening our workload or spending time with loved ones, our health care system is still required to run at full capacity.

A new study led by Institute of Health Policy, Management and Evaluation PhD student Lauren Lapointe-Shaw, has found that patients discharged from hospital during the two-week period over the holidays, are at a higher risk of death within the first 7 days of discharge, and are more likely to be readmitted to hospital within 30 days.
The study, published in The BMJ, also found that patients were less likely to receive a follow-up from their physician after discharge during the holidays versus other time of the year including the winter months of November and January.
“Based on our understanding of what might be occurring we can see there are a few possibilities,” said Lapointe-Shaw, who is also a general internist at Toronto General Hospital. “As with many services during the holidays, an individual’s family physician may be more difficult to access during this time, or patients themselves might be choosing to wait to schedule a follow-up because they are involved in holiday activities.”
Lapointe-Shaw and fellow researchers studied patient populations discharged into the community between 2002 and 2016 using data from the Institute of Clinical Evaluative Sciences. These patients were then compared to those discharged during the control periods of November and January with results indicating that those discharged the week before or the week after Christmas, regardless of age, were at an increased risk of death or hospital readmission. This also included a higher risk of returning to urgent care and emergency departments. Per 100,000 patients, there were 26 excess deaths, 188 excess re-hospitalizations and 483 excess visits to an emergency department that could be attributed to discharge over the holiday period.
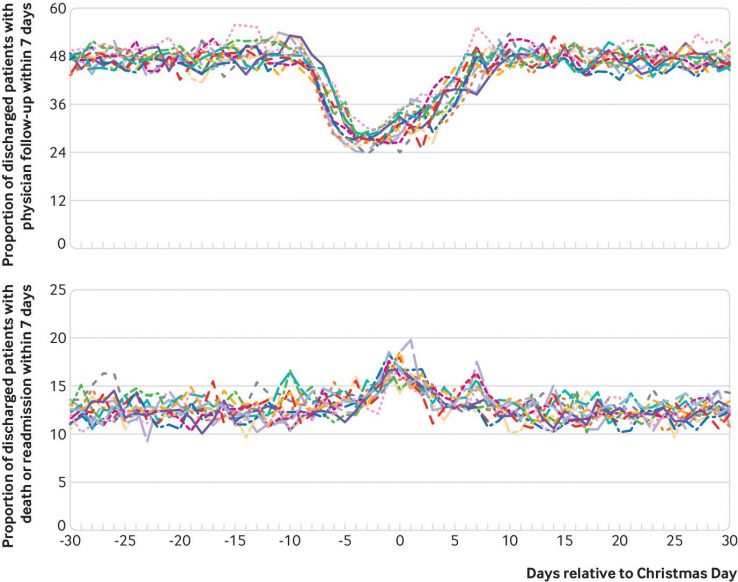
The “Christmas effect”, also shows the significant drop in patients each year who received a follow-up from their physician within 7 and 14 days of discharge. The drop off occurs right around Christmas day. While previous literature has looked at patients readmitted to hospital over weekends or those who were discharged over an isolated holiday, this is the first study to identify patients over a prolonged period of time where services may be less accessible.
“There were limitations to our study,” said Lapointe-Shaw, “and we can’t say for certain why some of these outcomes are being observed including why patients do not return for follow-ups. However, I think there is enough evidence in the study to encourage both health care providers and patients to pay closer attention to discharge planning.”
Discharge planning is a key focus of Lapointe-Shaw’s dissertation research. As a physician, she says her interest was piqued after witnessing the effects of good and inadequate discharge planning on her patients. Discharge planning often begins right as an individual is being admitted to a hospital, and includes determining patient stability, identifying all medications, and educating the patient on a plan to follow if new symptoms arise.
“As physicians, it is important for us to pay additional attention to discharge planning and for outpatient providers to ensure that patients don’t’ fall through cracks when resources are strained,” said Lapointe-Shaw. “ For Ontarians, I think it is great to see this level of interest in the issue of coverage in health care over the holidays. Changes have already been implemented in family physician clinics, and in the next few years we will need to see what kinds of results these changes have yielded in terms of our patient outcomes.”
For the rest of the public and for patients who may be discharged over the holidays, this study emphasizes the need to remain well-informed of their discharge plan and follow the recommendations of their physicians for additional check-ups as needed especially at this time of year.